Simulating the effect of transcranial brain stimulation
The long-lasting aftereffects of non-invasive transcranial direct current stimulation (tDCS) promise an alleviation of severe symptoms of diseases like depressive disorder or chronic pain. In a new modeling study, researchers from the Bernstein Center Freiburg suggest that the aftereffects observed in experiments may be a consequence of homeostatic network growth. Their model is based on the idea that the stimulation triggers a rearrangement of synaptic couplings among stimulated and unstimulated neurons, eventually leading to network remodeling and cell assembly formation.
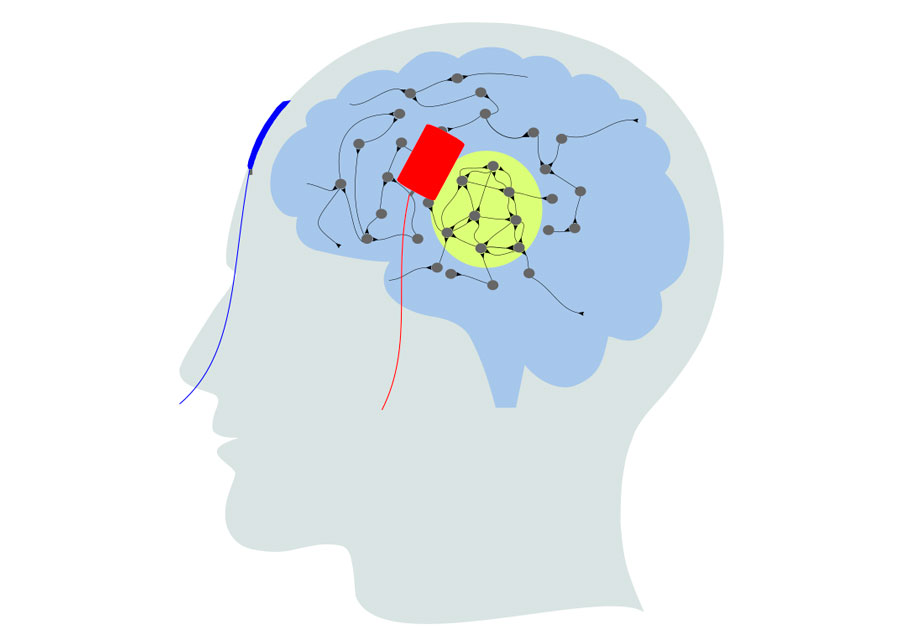
tDCS is applied by passing a weak current into the brain via pairs of electrodes attached to the scalp. The current is able to induce an electric field within the brain. Our model proposed a homeostasis based mechanism of its aftereffects, that the stimulation perpetuates the firing rate equilibrium at the most stimulated region (light yellow) and triggers synapse reorganization among the excitatory neurons. Eventually the connectivity is enhanced among the stimulated neurons and lead to cell assembly formation. © Bernstein Center Freiburg
/BCF/ Exposing the brain to very weak electric fields via head-mounted electrodes can have a positive impact in patients who suffer from brain-related diseases such as depressive disorder or chronic pain. Even after switching off the current, long-lasting positive effects have been reported for some patients, although the treatment results are variable, and their reproducibility is still rather poor. The method is nevertheless considered by many as a promising therapy option for the future. Understanding the cellular and systemic mechanisms underlying tDCS, therefore, is crucial to increase the confidence of doctors and patients, and to improve the broad applicability of the method in clinical practice.
New research by a team led by Prof. Stefan Rotter suggests that homeostatic structural plasticity might be key to understand how tDCS works. Using a new computational network model, the team has provided support for this hypothesis. In this model, the cortical tissue exposed to transcranial stimulation is conceived as a recurrent network of excitatory and inhibitory neurons. The idea: The stimulation perturbs the ongoing activity of certain neurons and changes their firing rates. This, in turn, influences how nerve cells are connected to each other, as “neurons that are too active strive to maintain a healthy firing rate by cutting off synaptic input that drives them too hard”, Han Lu, PhD candidate at the Bernstein Center Freiburg, explains.
Perturbing neuronal activity can lead to changes of network connectivity
On the other hand, a neuron grows new synapses, if its activity falls below a certain threshold. It simply seeks more input from others to restore its desired activity level. “This protocol of controlling growth is called homeostatic structural plasticity. The concept is well known to engineers, it works like a thermostat one finds in most heating systems”, Han Lu says. The new model assumes that tDCS triggers a homeostatic response of the network involving growth, decay and rearrangement of synapses among stimulated and unstimulated neurons. “This is eventually leading to network remodeling and cell assembly formation. Applied wisely, stimulation might also boost the self-repair of failing brain networks”, Han Lu postulates.
Using computer simulations, the researchers systematically tested the impact of various parameters of the stimulation, including electrode size and montage, as well as stimulation intensity and duration. Their results suggest that the stimulated population eventually reduces the number of excitatory synapses with unstimulated neurons, and new synapses among stimulated neurons are grown to form a cell assembly. Strong focal stimulation tends to enhance the connectivity within new cell assemblies, and repetitive stimulation with well-chosen duty cycles can increase the impact of stimulation even further. Han Lu adds: “Some of these stimulation patterns have previously been employed in tDCS experiments with human subjects. Our model appears to be able to make sense out of some unexplained observations made back then.”
She sums up: “Using theory and simulation, we have explored aspects of transcranial stimulation that might also be relevant for clinical practice. Currently, however, there is still a huge gap between theory and experiment, as it is not possible to measure the connectivity changes in experiments directly. This is what I would like to achieve in my PhD project. For the future, we hope that our work can help to improve the stimulation protocols in clinical applications.”
Text: Bernstein Center Freiburg
>> original press release
Original publication
Lu H, Gallinaro J, Rotter S: Network remodeling induced by transcranial brain stimulation: A computational model of tDCS-triggered cell assembly formation /Network Neuroscience/, 2019 https://doi.org/10.1162/netn_a_00097




